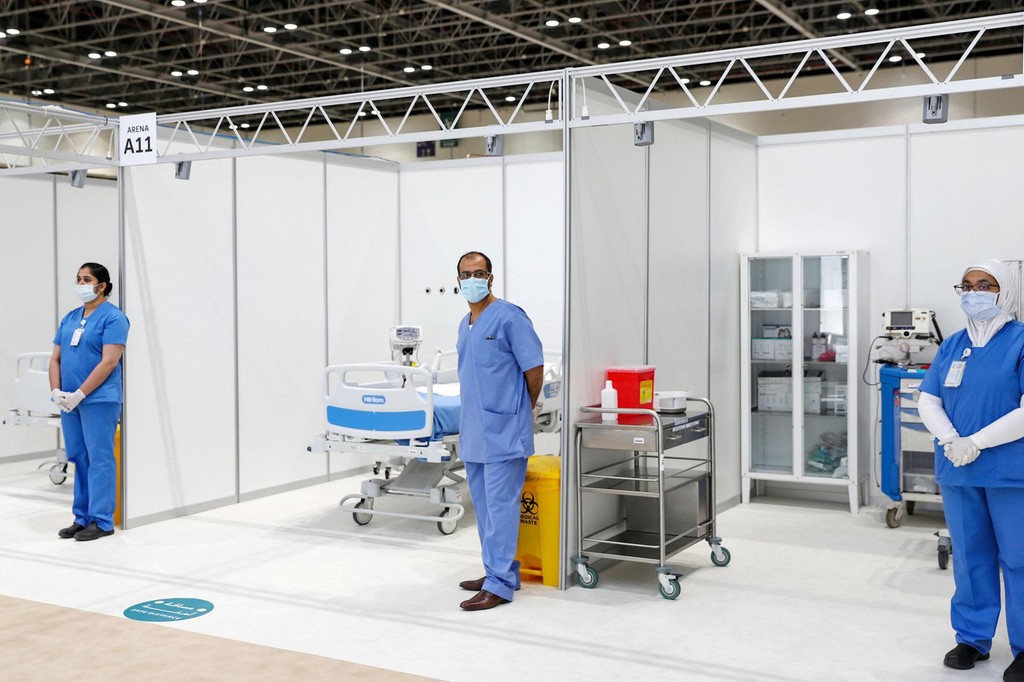
Field hospitals: A vital part of strengthening the health system response to COVID-19
In a pandemic response such as that experienced during COVID-19, government health authorities may reach capacity at the existing healthcare facilities and must enact emergency surge plans. Surge capacity is crucial to prevent health care worker infection and hospital collapse during an outbreak. Field or surge hospitals, so-called because they are designed to treat a surge in the number of patients needing care, are deployed in a wide range of scenarios including natural disasters and epidemic outbreaks and operation in these conditions requires adaptation to disaster medicine principles, while maintaining acceptable standards of care.
For healthcare authorities across the globe, including in the Middle East and North Africa (MENA) region, coming to terms with the enormity of the COVID-19 outbreak meant coming face to face with alarming hospitalisation rates and mortality rates. For examples, the Centres for Diseases Control and Prevention revealed that the overall cumulative COVID-19 hospitalisation rate in the United States was 98.4 per 100,000, with the highest rates in people aged 65 years and older (297.6 per 100,000) and 50-64 years (148.6 per 100,000). Meanwhile, data collected from 20 regions in Italy indicated that the average interregional case fatality rate was 7.5%, and the average ICU admission rate was 21.4%.
According to the World Health Organisation, what these experiences in the COVID-19 outbreak indicate is that ‘business-as-usual service delivery approaches’ are not sufficient to respond once a cluster of cases or widespread community transmission is registered and surge capacity will be needed. Creating surge capacity for acute and intensive care by repurposing or requisitioning of structures beyond the hospital setting to provide for excess patient numbers is vital to strengthening the health systems response to COVID-19 while maintaining essential hospital services.
Therefore, health authorities and healthcare organisations must understand what surge hospitals are and how they can plan for and establish them, including whom they should work with to do so. What steps need to be taken to safely and rapidly enact surge capacity? And who should be involved in planning, establishing, and operating surge hospitals?
A rapid response on a global level
While no single model exists for surge hospitals, the Advisory Board Group’s Global Forum for Health Care Innovators highlights three main categories of field hospitals. The first type of field hospitals is used for quarantining mild to moderate cases of Covid-19 using frequent monitoring and rapid referral protocols to transfer patients to existing hospitals if their conditions worsened. The second type is to create ICU capacity to care for critically ill Covid-19 patients, and the third type is intended for patients recovering from Covid-19. The latter no longer need to be in a critical care environment but can't yet return home.
Globally, there are some remarkable examples of how surge hospitals were built at a rapid pace. The first example of this was the 25,000-square-metre Huoshenshan Hospital, one of two new hospitals being built in just 14 days in the Chinese city of Wuhan. Another well-documented example is the Nightingale Hospital at Excel, London that provided up to 4,000 intensive care beds.
Across the MENA region, preventative measures to enhance capabilities to deal with a potential increase in COVID-19 patients also included the setting up of various surge hospitals across the region. In the UAE, the 29,000-square-metre field hospital in the capital’s Mohammed bin Zayed city set up with a capacity to treat 1,200 coronavirus patients is one example. At the same time, the authorities in Dubai converted the Dubai World Trade Centre into a field hospital that can house 3,000 coronavirus patients in a bid to ramp up the country’s capacity to treat people infected with COVID-19.
In Saudi Arabia, the Jeddah Centre for Exhibitions and Events reopened in June as a field hospital for Covid-19 patients to alleviate hospitals overrun with cases. Similarly, Kuwait’s authorities also set up a number of fields hospitals in areas such as the Farwaniya Governorate, Al-Mahboula, Al-Ardhiya and Mishrif, to name a few.
Meanwhile, the Egyptian authorities have recently mobilised to set up the country’s first official surge hospital set up on a plot of land behind the Ain Shams University with the capacity to treat 171 patients with 11 ICU beds. Ahead of this, Tunisian authorities announced the opening of the first field hospital to treat COVID-19 patient in the country with 84 beds.
Repurposing for the common good
Opening decommissioned or previously closed healthcare facilities is potentially a prudent option to handle the surge in capacity requirements during COVID-19. Strategic facility recommissioning and repurposing may help health organisations increase their testing capacity, dedicated and isolated space for COVID-19 treatment, or for other necessary functions critical to slowing the spread and optimising care. According to international design firm CannonDesign, an expedited recommissioning strategy must be developed that considers facility condition, safety and capability to handle new patients.
All decision-making should be based on relevant and accurate data in order to create a comprehensive understanding of facility assets ensuring that stated issues, recommendations, and action prioritisations reflect the as-observed existing conditions. Following the initial data collection steps, asset deficiencies should be assigned probable costs for mitigation. Once deficiencies are fully developed with recommendations and costs, they should be compiled into an asset summary report that contains relevant information for both administrators and facility managers.
Once all the data is gathered, an actionable execution strategy may be initiated. Lists of assets to be recommissioned or repurposed are built followed by developing projects based on the deficiency recommendations and costs, according to the CannonDesign guidelines.
Going beyond hospital beds
According to the Joint Commission on Accreditation of Healthcare Organisations, when planning for the potential use of a surge hospital, healthcare institutions need to consider their definition of surge capacity as more than just the number of available hospital beds. Instead, they need to think about their ability to handle a public health emergency by examining two additional types of resources inside their institutions: staffing and equipment.
Organisations also need to investigate pharmaceutical reserves in local pharmacies so they can have a ready supply of needed medications that last until additional supplies arrive. Also, communications systems and information technology should be in place so that the organisation can communicate with both internal staff and outside agencies. Another fundamental part of the planning process is the connectivity with community leaders and planning organisations to ensure compatibility with community thinking and functional initiatives.
All surge facilities must ensure that the care they provide is safe. Besides this, certain quality assurance processes must be followed in surge hospitals so that, for example, patients are identified, and drug errors do not occur. The longer a facility remains operational, the more demands must be made on both its environment of care and the process of care delivery to make sure they are in line with high standards of care. These demands can ensure that, while beneficial care may be given, substandard care is never allowed.
Strategy to reduce commissioning time for surge hospitals:
Commissioning equipment in an emergency (COVID-19) ITU surge hospital requires medical equipment engineers and technicians onsite, plus support staff to:
- Unpack the equipment and give a quick physical inspection for transit damage;
- Add it to the computerised asset management database;
- Take it to the designated bed space;
- Install it onto the bed, wall, drip stand, etc.;
- Connect the devices to electrical and/or compressed air and/or O2 supplies;
- Electrical safety testing (Class 1 patent connected equipment only);
- Functional testing (basic checks);
- Signing off on a database for use.
The armed forces or semi-skilled volunteers can perform the first four of these tasks, while tasks 5-8 require specialist EBME expertise.
Source: Clinical Services Journal
Case Study: Decommissioning The Nightingale Hospital in London’s Excel Conference Centre
The Nightingale Hospital at Excel, London, was set up in just ten days, with plans to provide up to 4,000 intensive care beds. The purchasing and commissioning equipment for the equivalent of 10 general hospitals required an estimated 112,500 hours of hands-on time to get the devices to the patients. Each intensive care bed space requires, on average, around 15 pieces of equipment to support a single patient. For London’s Nightingale Hospital, this equates to over 60,000 pieces of equipment – some of which is highly specialised – such as ventilators, humidifiers and patient warmers.
Once the pandemic subsides, and the field hospitals are no longer required, the question arises of what should happen to all the extra medical equipment procured. How should it be decommissioned? There is also the question of what should happen to ensure the country is equipped and better prepared to deal with future outbreaks of this kind.
According to the Clinical Services Journal, the major lesson to be learnt for the future is that proper pandemic planning and putting real contingencies in place, in terms of medical equipment, would be at a fraction of the cost. Using large exhibition spaces is a good model for getting field hospitals up and running, but the challenge has been “having the equipment ready to go”. Going forward, a strategy must be developed to ensure contingency in the future.
It would also be useful to have a database for emergency equipment that is used by all hospitals in the country, in the event of a pandemic or disaster. Hospital directors who are already responsible for overseeing emergency responses, such as terrorist attacks, should also be given responsibility for ensuring there is sufficient contingency stock of equipment during a pandemic. Similarly, a lot could be learned a lot from the military and the way they respond to incidents, particularly in terms of their use of centralised libraries.
A good problem to have
The question on many people’s minds is what happens to temporary surge facilities created in response to COVID-19 once the need for the space returns to pre-pandemic levels? Today, with virus infections slowing down or falling short of worst-case prediction, many surge hospitals across Europe, the MENA region and the United States are seeing diminished use, and many are shutting down.
As the makeshift medical centres were built in anticipation of worst-case policy measures, some argue that this is a good problem to have because it's a sign the deadly disease was not nearly as cataclysmic as it might have been. With further waves of COVID-19 possible, and until a vaccine is developed or most of the world’s population is infected, many of these facilities will now be kept on standby, and some could even be repurposed as testing sites or recovery centres.
About Arab Health
Arab Health is the largest healthcare event in the Middle East and is organised by Informa Markets. Established in 1974, Arab Health provides a platform for the world’s leading manufacturers, wholesalers and distributors to meet the medical and scientific community in the Middle East and subcontinent.
The upcoming edition of the event is expected to welcome the healthcare industry to view the latest healthcare innovations, products and services, and experience the highest quality Continuing Medical Education (CME) conferences for medical professionals in the region.
Interested in participating in Arab Health?
If you have any other queries, email us on [email protected]